You’ve been outside for hours. Your head is pounding, your vision is spotty, and even though you’re drenched in sweat, you can’t cool down. You don’t know if it’s just the heat or something more serious. Knowing the difference between dehydration, heat exhaustion, and heatstroke could save your life.
Key Takeaways
- Heat exhaustion effects include heavy sweating, dizziness, weak pulse, and muscle cramps caused by fluid and salt loss in hot conditions
- It’s more serious than dehydration but differs from heatstroke by the absence of confusion or altered mental status
- Quick cooling, rest, and rehydration prevent progression to life-threatening heatstroke
Heat exhaustion is your body’s response to too much heat, fluid loss, and salt loss. It’s more serious than simple dehydration but not yet heatstroke. It shows up as heavy sweating, weakness, and exhaustion that feels out of proportion to what you did. Understanding heat exhaustion effects, how it differs from other heat related illnesses, and when to get help can stop a bad episode from becoming an emergency.
1. How to Tell If It’s Heat Exhaustion?
Heat exhaustion doesn’t always announce itself clearly. You feel like someone unplugged your battery. You’re hot but clammy, light-headed when you stand, and your legs are shaky. Your pulse is racing, but you feel wiped out. Common signs of heat exhaustion include:
- Heavy sweating with cold, clammy, or pale skin
- Dizziness, pounding headache, or feeling faint
- Nausea or vomiting
- Painful muscle cramps—often the first warning sign
- Fast but weak pulse
- Overwhelming fatigue that feels too extreme for what you were doing
- Intense thirst even if you’ve been drinking water
Your body temperature typically rises to between 101 and 104 degrees Fahrenheit. Symptoms can start suddenly or build gradually, especially during long exercise or work in the heat. Some people also feel irritable, have trouble coordinating movements, and notice decreased urination.
These heat exhaustion symptoms are your body’s alarm system—designed to make you stop, find shade, and drink fluids before the situation becomes dangerous.
2. What Heat Exhaustion Does to Your Body?
The effects of heat exhaustion come from a cascade of physical changes when your body can’t release heat fast enough.
When exposed to heat, your body pushes more blood toward your skin and produces sweat to cool down. This can double your heart’s workload. The problem starts when sweating drains your fluid levels. As blood volume drops, less blood returns to your heart. Blood vessels in your skin expand to help with cooling, which further reduces blood available to your core organs.
This creates the main heat exhaustion effects: Your blood pressure drops. Blood flow to your brain and muscles decreases, causing dizziness, weakness, wobbly legs, and faintness. Your heart rate jumps to maintain circulation—this is why your pulse feels fast but weak.
The loss of electrolytes from sweating, especially sodium and potassium, triggers painful muscle cramps. Your kidneys also feel the strain as heat stress reduces blood flow and activates hormones that concentrate your urine.
These are warning effects, not yet permanent damage. Heat exhaustion is your body’s emergency brake—forcing you to stop, cool down, and rehydrate before real organ damage occurs.
3. What Causes Heat Exhaustion?
Heat exhaustion happens when your body’s cooling system is overwhelmed. The causes of heat exhaustion combine with a hot environment, high humidity, physical exertion, and insufficient fluid or salt intake—your body can’t release heat fast enough. Common scenarios:
- Outdoor sports, especially before acclimatization
- Construction or warehouse work in summer
- Yard work or home projects in heat
- Long hikes or runs in hot, humid climates
- Crowded spaces without air conditioning
- Travel from cool to hot climates
High-risk groups for heat-related illness:
- Infants, children under four, and adults over sixty-five
- People taking diuretics, beta-blockers, antihistamines, or certain antidepressants
- Those with obesity, heart disease, diabetes, or kidney disease
- Anyone new to hot climates or facing sudden heat waves
- Anyone with previous heat exhaustion or heatstroke
The heat index (temperature plus humidity) matters more than temperature alone. Deaths can occur when the heat index is only eighty-five to ninety degrees. When it hits ninety-one degrees or higher, precautions are essential.
Athletes know that even fit, healthy people are vulnerable when pushing hard in the heat without proper hydration and acclimatization.
4. How Long Does Heat Exhaustion Last?
The recovery timeline for heat exhaustion depends on how quickly you act, how severe the episode was, and whether you give your body the rest it needs.
The First 24–48 Hours
With quick cooling and rehydration, many people feel significantly better within thirty minutes to a few hours. Extreme fatigue and dizziness ease first, followed by improvements in nausea and muscle weakness. Common short-term after-effects:
- Ongoing fatigue and muscle soreness for one to two days
- Mild headache or brain fog
- Lower tolerance for heat and physical work
- Sleep disruption
Most people need at least 24 to 48 hours to feel normal and should avoid heat exposure and strenuous activity during this time.
Long-Term Consequences of Repeated Heat Illness
Severe or repeated episodes can stress your heart, kidneys, and nervous system. Studies show that heatstroke survivors may develop lasting immune system changes, with higher risks of chronic heart disease and kidney disease later in life.
Heat stress-related kidney injury contributes to an epidemic of chronic kidney disease in work settings. Research confirms heatstroke is linked to long-term organ problems and increased vulnerability to future heat illness.
Frequent heat exhaustion episodes signal you need to change how you handle heat—the effects can be lasting and serious, especially with underlying health conditions.
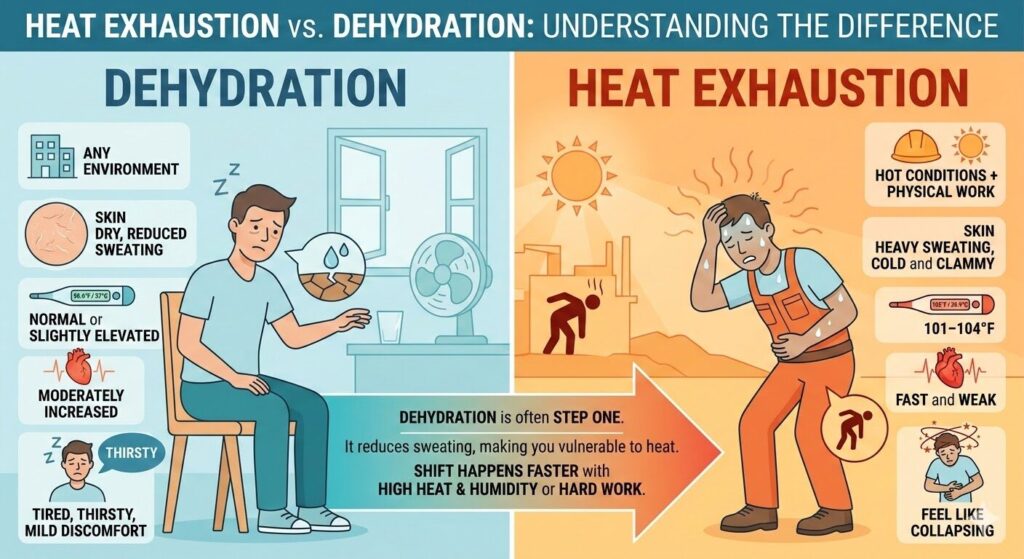
5. Heat Exhaustion vs Dehydration
Many people confuse these conditions, but they’re different. Dehydration is a fluid deficit that can happen anywhere—even in an air-conditioned room. Heat exhaustion requires both fluid loss and heat stress.
| Feature | Dehydration | Heat Exhaustion |
| Setting | Any environment | Hot conditions + physical work |
| Skin | Dry, reduced sweating | Heavy sweating, cold and clammy |
| Temperature | Normal or slightly elevated | 101–104°F |
| Pulse | Moderately increased | Fast and weak |
| Severity | Tired, thirsty, mild discomfort | Feel like collapsing |
Dehydration is often step one. It reduces your body’s ability to sweat and maintain normal temperature, setting the stage for heat exhaustion when you’re exposed to hot conditions. The shift happens faster in high heat and humidity, during hard work, or when you’re not used to the environment.
Understanding dehydration and heat exhaustion helps you respond correctly as conditions worsen.
6. Heat Exhaustion vs Heatstroke
The line between heat exhaustion and heatstroke is the difference between a serious warning and a life-threatening emergency.
| Feature | Heat Exhaustion | Heatstroke |
| Core temperature | 101–104°F | ≥104°F and rising rapidly |
| Skin | Heavy sweating; cold, clammy | Hot, dry or sweating stopped |
| Mental status | Tired, dizzy but alert | Confusion, seizures, unconsciousness |
| Pulse | Fast, weak | Fast, strong |
| Risk | Serious; needs cooling | Medical emergency |
Mental status is the critical difference. With heat exhaustion, you stay alert and aware. Heatstroke causes confusion, slurred speech, seizures, or loss of consciousness—the nervous system is failing.
Heatstroke kills thirty-three to eighty percent of people without fast treatment. The brain is especially vulnerable, and the heart, kidneys, and liver can suffer permanent damage.
Call 911 immediately if you see: confusion, collapse, seizures, very hot skin, or stopped sweating. Don’t try treating heatstroke symptoms at home—it requires emergency medical care.
7. How to Treat Heat Exhaustion?
Recognizing heat exhaustion and acting immediately can prevent the condition from becoming heatstroke. The treatment is straightforward, but it must be done correctly and without delay.
- Move to a cool, shaded, or air-conditioned area immediately. Get out of the sun and away from the heat source.
- Lie down and raise your legs slightly to help restore blood flow to your core and brain.
- Remove excess or tight clothing, including shoes and socks, to let your body release heat more easily.
- Start active cooling right away. Apply cool, not ice-cold, wet cloths or compresses to your skin, focusing on your head, face, neck, armpits, and groin—areas where blood vessels are close to the surface. Mist your skin with water and use a fan to encourage evaporative cooling. Avoid ice baths or extremely cold water, which can cause shivering and actually raise your core temperature.
- Sip cool water or a sports drink with electrolytes if you are awake and not vomiting. Drink small, frequent sips rather than gulping large amounts, which can trigger nausea. Avoid alcohol and very sugary drinks, which can make dehydration worse. The goal is steady, gradual rehydration while your body cools.
Seek urgent care or emergency room evaluation if your symptoms of heat exhaustion don’t improve within one hour of cooling and drinking fluids. If you are vomiting repeatedly or can’t keep fluids down, you need IV fluids and electrolyte monitoring that can only be provided in a medical setting.
Certain people should seek care sooner. If you have heart disease, kidney disease, are pregnant, very young, or an older adult, get a medical evaluation at a lower threshold. Medical care adds the ability to give IV fluids, fix electrolyte imbalances, monitor vital signs continuously, and check labs for kidney function, muscle breakdown, and sodium or potassium levels.
It’s critical to understand when the situation has moved beyond heat exhaustion. Any signs of heatstroke—confusion, seizures, loss of consciousness, very hot dry skin, or a core temperature at or above 104 degrees Fahrenheit—require you to call emergency services, not a mobile or home IV service. Heatstroke is a hospital emergency, not a condition that can be managed at home.
8. How to Prevent Heat Exhaustion?
Prevention works better than treatment. Once you’ve experienced heat exhaustion, your body may be more vulnerable to future episodes, which makes developing heat-smart habits essential.
Before Heat Exposure
Check the heat index, not just the temperature. The heat index accounts for humidity, which drastically affects your body’s ability to cool through sweat evaporation. At a heat index of ninety to one hundred five degrees, sunstroke, muscle cramps, and heat exhaustion are possible with long exposure or physical activity. At one hundred five degrees and above, heatstroke becomes likely.
Pre-hydrate the day before and the morning of any heavy work. Set phone alerts to remind yourself to drink. Plan your hardest work or exercise for the cooler parts of the day—early morning or evening.

During Heat Exposure
Drink on a schedule rather than waiting for thirst. Aim for about four cups of water per hour in moderate to high-risk conditions, sipping every fifteen to twenty minutes. Thirst is a late sign of dehydration, and by the time you feel thirsty, your performance and heat tolerance are already reduced.
Take regular shade or air-conditioned breaks. Continuous work in the heat is not advisable—you must give your body periodic rest to cool down. Wear light-colored, loose, breathable clothing and a hat. Sunburn hurts your body’s ability to cool itself, so use broad-spectrum sunscreen with SPF fifteen or higher.
Use a buddy system when working or exercising in teams. A partner can recognize early signs of heat exhaustion in you that you might miss, get help, and call for emergency help if needed.
Build Heat Tolerance
Your body adapts through repeated heat exposure—starting to sweat earlier, producing more sweat, losing fewer electrolytes, and maintaining lower core temperature. Most adaptations occur within four to seven days, with full optimization in two weeks.
New workers should limit heat exposure to twenty percent on day one, increasing by twenty percent daily. Acclimatization fades after a week away from heat but returns quickly.
Build fitness gradually in hot weather. If you struggle with heat, review medications with your doctor. Watch for early warning signs and respond immediately by stopping, finding shade, and rehydrating effectively.
Whether you’re dealing with Texas heat, Atlanta’s humidity, or Vegas temperatures, the principles remain the same: hydrate proactively, cool down regularly, and respect your body’s limits.
Heat exhaustion is your body’s urgent warning to stop, cool down, and rehydrate before the situation becomes life-threatening. Recognizing the symptoms, understanding how heat exhaustion effects differ from dehydration and heatstroke, and knowing how to respond can prevent serious complications. If you’re recovering from heat exhaustion or struggling with heat-related symptoms, rest and rehydration are essential—and in many cases, IV fluids can help restore your body’s balance faster and more effectively than drinking fluids alone.