Key Takeaways
- Most IV therapy side effects, like bruising and nausea, resolve within hours without treatment.
- Serious complications are uncommon but need quick recognition and response.
- Pre-treatment screening is the most effective way to prevent IV therapy side effects before they start.
Your IV drip is running, and suddenly your arm feels cold, your stomach turns, or the needle site starts to ache. Is that normal, or is something going wrong?
For the millions of people who get IV infusions each year, these moments of doubt are common. Most IV therapy side effects are mild and pass quickly, but a small number point to something that needs immediate attention. The gap between simple discomfort and real danger often comes down to knowing what to watch for.
This guide breaks down every IV drip side effect by severity so you can understand what your body is telling you, spot which reactions are routine, and recognize the warning signs that call for medical help.
1. Most IV Therapy Side Effects Are Mild and Temporary
If you’re new to what IV therapy involves, your body is not used to receiving fluids through a vein. A catheter is a foreign object, the fluid is cooler than your blood, and the delivery rate is faster than anything your digestive system would allow. That mismatch explains nearly every mild reaction on this list, and it also explains why they pass so quickly once your body adjusts.
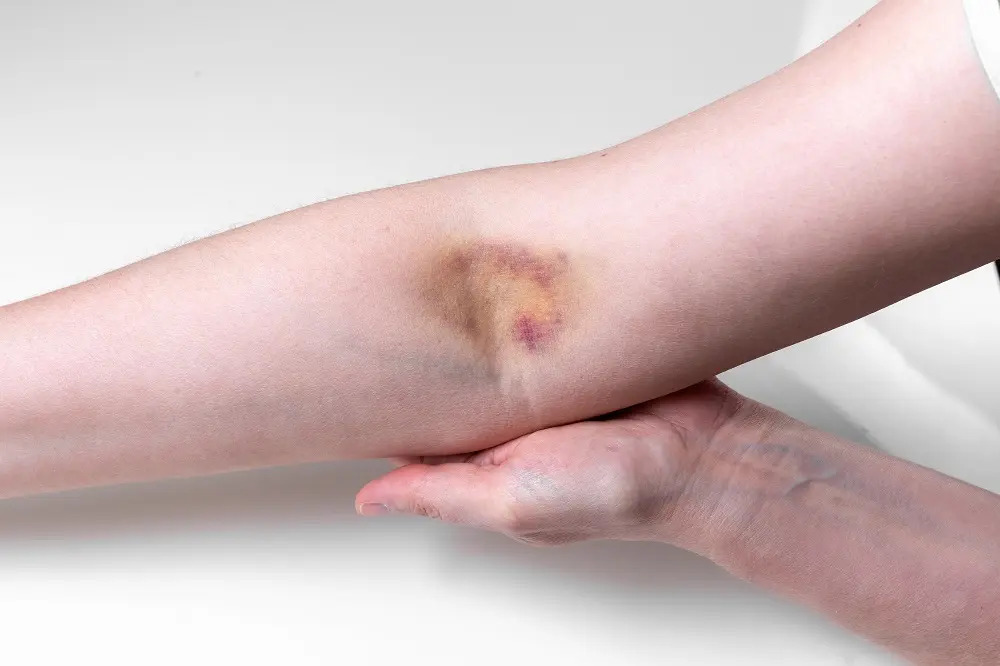
Bruising, Soreness, or Redness Around the Needle Site
This is the most common reaction to any IV infusion, and it works the same way as bruising from a routine blood draw. When the catheter enters the vein wall, small amounts of blood can leak into the surrounding tissue and form a minor bruise. Slight catheter movement during the infusion can also irritate the inner lining of the vein, causing redness and tenderness at the site.
This soreness usually clears up within 24–48 hours without any treatment. A cool compress applied right after the infusion and keeping your arm raised can reduce swelling and speed recovery.
Watch for redness that starts tracking upward along the vein instead of staying near the needle site. That pattern, especially with growing warmth or hardness along the vein, points to a different condition called phlebitis, covered further in this article.
Nausea or Lightheadedness During the Drip
Feeling queasy or slightly dizzy during an IV infusion usually comes from rapid fluid delivery. When a large volume of fluid enters the bloodstream quickly, the sudden increase in blood volume triggers sensors in the cardiovascular system. This can set off a vasovagal response, marked by lightheadedness, pale skin, and nausea. Certain vitamins add to the effect. High-dose B-complex and vitamin C are known irritants that can cause nausea when infused at faster rates.
This reaction happens more often in first-time recipients and in people who arrive on an empty stomach. Fasting lowers both blood sugar and baseline fluid volume, making the body more sensitive to rapid shifts. The fix is simple: the provider slows the drip rate, you lie back and focus on steady breathing, and the feeling typically passes within 5–10 minutes.
One key distinction matters here. Nausea by itself is almost always harmless. Nausea paired with hives, facial swelling, or any trouble breathing is a sign of an iv therapy allergic reaction and needs immediate escalation.
Headache or Fatigue After Treatment
A headache after an IV session can catch people off guard, but the cause is straightforward. IV fluids shift your fluid balance and electrolyte levels rapidly. Even slight overhydration can dilute sodium in the blood, a condition called dilutional hyponatremia, which commonly shows up as a headache. High-dose vitamin C infusions above 10 grams are also linked to headache as a known minor side effect.
Some people also feel a temporary energy dip after treatment. Processing a concentrated dose of vitamins and minerals takes metabolic effort, similar to the recovery your body goes through after hard exercise. Rest and drinking water resolve these symptoms within 2–4 hours in most cases. If a headache lasts beyond 24 hours or comes with visual changes or confusion, contact your provider.
Feeling Cold or Tasting Something Metallic
Standard IV solutions are stored at room temperature, roughly 20–22°C, well below your core body temperature of 37°C. As that cooler fluid enters the bloodstream, temperature sensors in the veins pick up the difference and create a cold sensation. This is basic physics, not a complication. A warm blanket and a slower drip rate make a clear difference.
A metallic taste during the infusion is equally harmless. Minerals like zinc and magnesium, along with vitamin C, reach taste receptors through the bloodstream within seconds. The metallic taste from vitamin C is especially well-documented in clinical IV vitamin therapy. Both feelings fade within minutes once the drip rate slows or the infusion finishes, and neither needs any treatment.
2. When IV Therapy Side Effects Turn Serious
Everything above falls into the “uncomfortable but harmless” category. The complications below are different. They involve fluid going where it should not, veins becoming inflamed, immune systems overreacting, or bacteria finding an entry point. Each one is uncommon with a qualified provider, but each one also has a narrow window where recognizing what is happening changes the outcome. Understanding these risks of IV therapy is what separates a prepared patient from a panicked one.
Your Arm Swells or Feels Puffy Around the IV Site (Infiltration)
IV infiltration happens when the catheter shifts out of place and the fluid leaks into surrounding tissue instead of flowing into the vein. It is 1 of the most common IV infusion side effects in clinical settings. Pediatric studies report complication rates, including infiltration, ranging from 18.9–71% in hospitalized populations, while adult studies show minor problems in about 11.3% of infiltration cases.
You will notice swelling and puffiness around the insertion site. The skin may feel cool and tight, and the drip may slow or stop. The response is immediate: stop the infusion, remove the catheter, raise the limb, and apply a compress. Clinical data show that 87.5% of consults for infiltration recommend elevation with compresses and close monitoring as the standard approach. Proper catheter securing and avoiding insertion at joint bends are the main preventive steps.
The Vein Becomes Red, Warm, or Hard to the Touch (Phlebitis)
Phlebitis is inflammation of the vein wall, triggered by 3 separate causes: physical irritation from the catheter, chemical irritation from acidic or concentrated solutions, and bacterial infection. A 2024 study found that phlebitis remains a major cost driver and patient safety concern in peripheral IV catheter use. Key risk factors include female sex, large catheter size, and certain high-risk medications.
The signature symptoms are redness tracking along the vein, warmth, tenderness, and a cord-like hardness you can feel under the skin. Physical phlebitis is managed by stabilizing the catheter, applying heat, and raising the limb. Chemical phlebitis requires switching to a slower rate or a more diluted solution. Infectious phlebitis calls for immediate catheter removal and monitoring for spreading infection. Recovery can take several days depending on severity.
The incidence numbers below show just how much phlebitis rates vary depending on the clinical setting, the catheter used, and the protocols in place.
| A single hospital cut its phlebitis rate from 96% to 55% just by improving IV insertion technique, with no new equipment or drugs. Provider training is the most powerful prevention tool available. |
You Feel a Burning Sensation and the Skin Changes Color (Extravasation)
Extravasation is a more severe form of infiltration. Where infiltration involves harmless fluids leaking into tissue, extravasation involves vesicant agents, medications that cause direct tissue damage when they escape the vein. Symptoms include intense burning or stinging at the site, skin that shifts from pale to red to blistered, and in severe cases, tissue death.
The response is to stop the infusion right away without flushing the line. Specific antidote treatments may need to be given before the catheter is removed. In the context of wellness IV drips, true extravasation is rare because vesicant agents are not typically used. However, high-dose vitamin C can cause significant local tissue irritation if it leaks outside the vein, so the distinction still matters.
Hives, Throat Tightening, or Difficulty Breathing (Allergic Reaction)
An IV therapy allergic reaction can range from a mild skin rash to life-threatening anaphylaxis. IV solutions contain active ingredients, stabilizers, preservatives, and carrier fluids, any of which can trigger an immune response. Because IV delivery skips the digestive tract entirely, the full load of potential allergens hits the immune system all at once.
Reactions follow a clear severity scale:
- Mild: Localized itching and hives. Treatable with antihistamines and slowing or stopping the drip.
- Moderate: Widespread flushing, swelling, and mild airway tightening. The infusion must stop, followed by antihistamines and corticosteroids.
- Severe (anaphylaxis): Rapid airway closure and a drop in blood pressure. Requires an immediate injection of epinephrine into the muscle.
Patients with G6PD deficiency face a higher risk of red blood cell breakdown specifically with high-dose IV vitamin C.
Shortness of Breath or Rapid Heartbeat from Too Much Fluid Too Fast
What happens if iv fluids are given too fast is a question with serious clinical weight. Fluid overload occurs when IV fluids enter the body faster than the heart and kidneys can handle, causing excess fluid to build up in the lungs and surrounding tissue. In a 2-year study, 21% of IV fluid therapy patients developed fluid overload, and 64% of those showed signs of fluid in the lungs on chest imaging.
Fluid overload symptoms include sudden shortness of breath, rising blood pressure, swollen hands and feet, puffy eyes, and in severe cases, coughing up pink or frothy fluid. Patients with heart failure, chronic kidney disease, and elderly adults are far more vulnerable. The response involves stopping or slowing the infusion, raising the head of the bed, giving supplemental oxygen, and potentially prescribing diuretics. This is why drip rate control and thorough pre-treatment screening are non-negotiable safety steps.
Redness, Pus, or Fever at the IV Site (Infection)
Catheter-related bloodstream infection happens when bacteria enter through the skin puncture, the catheter hub, or contaminated IV tubing and reach the bloodstream. Research shows that peripheral IV catheter-associated bloodstream infections make up 13–23% of all catheter-associated bloodstream infections. A meta-analysis found a 14% death rate in these cases, and a 2025 JAMA Network Open study showed that infection risk jumps sharply after day 3 of catheter use, with an adjusted odds ratio of 13.55.
Symptoms include spreading redness and growing warmth around the site, pus or drainage, and fever typically appearing within 24–48 hours after the infusion. The response is to remove the catheter immediately, culture the drainage, and start antibiotic therapy while watching for signs of sepsis. This risk is higher in non-clinical wellness settings where sterile protocols may be less strict.
| A 2025 Yale/JAMA Internal Medicine study found that over 85% of IV hydration clinics recommended specific IV cocktails without asking about the customer’s medical history, and 0 of the 255 clinic websites reviewed disclosed risks like infection or allergic reactions. |
3. Rare Complications That Require Emergency Response
The IV therapy complications above are uncommon. The ones below are genuinely rare, but they share a common trait: the faster you recognize them, the better the outcome. Even a few minutes of delay can change the clinical picture, which makes awareness the single most valuable thing you can carry into any IV session.
Air Entering the Bloodstream (Air Embolism)
An air embolism occurs when air enters the IV line, usually during catheter insertion, removal, or when IV bags are being swapped, and travels into the veins. Research shows that as little as 2–3 mL of air in the brain’s blood supply can be fatal, and an accidental 10 mL dose can cause serious harm.
Symptoms include sudden shortness of breath, persistent coughing, chest pain, rapid heartbeat, confusion, and a feeling of impending doom. The emergency response is to seal the source of air, place the patient on their left side with the head lowered, give 100% oxygen, and call emergency services right away. Modern IV equipment with air-detection sensors has made this event extremely rare, and fully priming IV tubing before use is the main preventive step.
Blood Clot Forming in the Vein (Thrombophlebitis)
Thrombophlebitis combines vein inflammation with blood clot formation in the affected vessel. It is most common after prolonged or repeated IV catheter use in the same vein. Symptoms include a painful, swollen vein that feels hard and warm to the touch.
Superficial thrombophlebitis at an IV site is typically treated with warm compresses, anti-inflammatory medication, and catheter removal. If deep vein thrombosis is suspected based on major limb swelling and skin discoloration, blood-thinning therapy and specialist evaluation are needed.
Nutrient Overload from Frequent Wellness Drips
This is the complication most specific to the growing wellness IV trend, and the 1 most readers will not have thought about. IV delivery bypasses the digestive tract’s natural absorption limits entirely. What the gut would normally block or flush out, the bloodstream absorbs in full.
Fat-soluble vitamins A, D, E, and K build up in fat and liver tissue with repeated infusions because, unlike water-soluble vitamins, the body cannot simply excrete the excess. Electrolyte imbalances from frequent IV drips can show up as muscle weakness, confusion, and irregular heartbeat. Potassium overdose specifically carries the risk of fatal heart rhythm problems. Cleveland Clinic experts warn that vitamin toxicity from excessive IV dosing can lead to heart damage, stroke, or even death in worst-case scenarios.
A PubMed scoping review of high-dose IV vitamin C found over 932 adverse events across 2,801 participants, including kidney damage from oxalate buildup and red blood cell breakdown in G6PD-deficient patients. Medical experts warn that without lab work and a full medical history, providers may unknowingly push nutrient levels well past safe limits. Pre-treatment health screening and provider-guided frequency recommendations are the most effective safeguards against nutrient overload.
4. Why Some People Are More Likely to Experience Side Effects
The same IV drip can produce completely different reactions in 2 people sitting side by side. The difference is rarely the formula. It is almost always the health profile of the person receiving it, which is why a 5-minute screening conversation before treatment carries more protective value than most people realize.
Patients with heart failure or chronic kidney disease cannot handle extra fluid efficiently, making fluid overload a real concern with any IV load. Elderly patients tend to have more fragile veins, which raises the chance of infiltration and bruising, while their slower metabolism affects how fast the body processes fluids. Immunocompromised individuals face higher infection risk even when sterile technique is followed carefully. Pregnant women need adjusted IV formulas and closer monitoring, especially during the first trimester.
First-time IV recipients are a unique risk group because they have no established tolerance baseline. Anxiety about the procedure can amplify vasovagal responses, adding to lightheadedness and nausea. People getting IV therapy in non-clinical wellness settings may also face greater risk from reduced medical oversight, potentially lax sterile protocols, and no pre-screening. So is IV therapy safe? For most healthy adults with a qualified provider, yes. For people in higher-risk categories, safety depends entirely on thorough screening and clinical oversight.
If any of these categories describe you, share that information with your provider before treatment begins.

5. When to Get Emergency Help After IV Therapy
Most side effects resolve on their own or with minor adjustments during the session. A small number of symptoms, however, signal something that cannot wait. If any of the following appear after an IV infusion, call 911 or go to the nearest emergency room immediately.
- Difficulty breathing or chest tightness
- Swelling of the face, lips, or throat
- Widespread hives or a rapid-onset rash
- High fever with spreading redness at the IV site
- Sudden confusion, rapid heartbeat, or fainting
- Severe burning or visible tissue discoloration at the IV site
These symptoms can signal anaphylaxis, fluid overload, bloodstream infection, or air embolism, all of which need urgent medical care. Acting quickly is always the right call.
Most IV therapy side effects are mild, predictable, and resolve within hours. Serious complications like infiltration, phlebitis, and allergic reactions are far less common and almost always manageable when caught early. The key is knowing what to expect at every severity level and choosing a provider whose protocols, from pre-treatment screening to sterile technique, are built to keep you safe. If you are considering IV therapy or want a provider you can trust, Mobile IV Medics delivers registered-nurse-administered treatments with thorough health assessments built into every visit.








